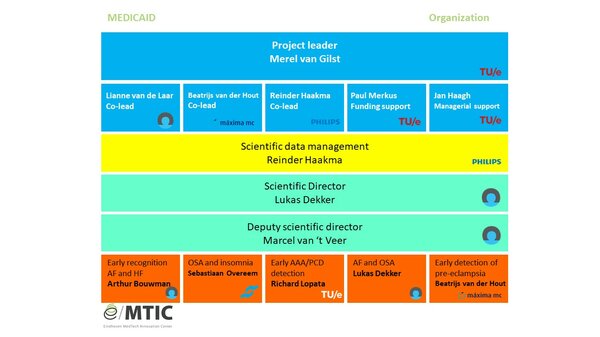
Merel van Gilst – Project leader
MEDICAID – e/MTIC mini-program
Within the Medtech solutions for Earlier Detection of CArdiovascular Disease (MEDICAID) project, 10 PhD students and 1 postdoc work on technological advances in unobtrusive sensing, monitoring and data analysis to enable earlier recognition, mitigate progression and improve treatment of cardiovascular disease.
The project consists of 5 work packages: WP1: Early recognition of Atrial Fibrillation and Heart Failure; WP2: Comorbid OSA and Insomnia: Cardiovascular based diagnosis and phenotyping; WP3: Early detection of preeclampsia; WP4: Diagnosis and management of Atrial Fibrillation compounded by Obstructive Sleep Apnea; WP5: Automated analysis of abdominal aortic aneurisms (AAAs) by means of ultrasound. As such the project covers the main three research area’s of e/MTIC. MEDICAID involves a close collaboration between engineering and clinical experts.
The general approach is to co-develop novel technological solutions in a controlled clinical environment, and to subsequently refine and validate them in extramural and at-home settings, immediately followed by deployment in the healthcare system. The program will run for approximately five years. Consortium: Philips, Maxima Medical Centre, Catharina Hospital, Kempenhaeghe, TU/e
Federica Sammali (WP1)
Project: Early recognition of Atrial Fibrillation (AF) and Heart Failure (HF)
This project covers some cardiovascular conditions, such as atrial fibrillation (AF) and heart failure (HF) in clinical as well as extramural settings. The project is complementary to and leverages on several ongoing projects within e/MTIC seeking to leverage technological advances in unobtrusive sensing, monitoring and data analysis to enable earlier recognition, mitigate progression and improve treatment of cardiovascular disease. This way, controlling and monitoring symptoms can allow for prevention of cardiac dysfunction with subsequent heart failure. Unobtrusive wearable technologies (incl. wristbands) are combined with user-friendly patient experience capturing solutions (incl. patient diaries) that have been developed within e/MTIC in recent years. This project aims at a) validating and refining these technologies for self- monitoring outside the hospital, and b) integrating them into a reliable, patient-friendly solution for timely detection of AF episodes and of HF deterioration by combining objective and subjective self-monitoring information with information acquired in the clinical setting. The close collaboration between engineering at TU/e and at Philips as well as clinical experts at Catharina Hospital, gives me the opportunity to closely work with people with different expertise in a multidisciplinary environment.
Bernice Wulterkens (WP2)
Comorbid OSA and Insomnia: Cardiovascular based diagnosis and phenotyping
Obstructive sleep apnea (OSA) and insomnia are the most prevalent sleep disorders. Today, there is growing attention for the co-occurrence of these disorders, which is also called COMISA. However, diagnosis and treatment are challenging, as both disorders share similar symptoms. My PhD project is about the identification of characteristics of COMISA. We will set up a large scale, longitudinal clinical study in collaboration with the Amphia hospital in Breda. We will measure long-term sleep in patients with a suspicion of OSA, using modern unobtrusive home-assessment techniques. By combining objective and subjective sleep measurements, we aim to get a better understanding of COMISA and to find predictors for the disorder, which will improve diagnosis and treatment.
The e/MTIC ecosystem gives me the opportunity to work with specialists from Kempenhaeghe, TU/e and Philips research who have a lot of experience in different areas of sleep research. In addition, it is very interesting to learn about the collaboration between the different institutes, while keeping their own interests in mind. In the past six months, I already learned a lot from the start of this PhD project, and I am sure that many opportunities and chances are waiting for us in the upcoming years.
Maretha Bester, Suzanne Moors (WP3)
Project: Early detection of preeclampsia
This MEDICAID work package focuses on perinatology. It is a collaboration between the Department of Electrical Engineering (BM/d, SPS) at TU/e, the Department of Obstetrics and Gynecology at Máxima MC, Veldhoven and Department of Family Care Solutions at Philips Research.
Pregnancy is a period of continuous cardiovascular change, partly mediated by the autonomic nervous system (ANS). However, in cases of preeclampsia (a hypertensive pregnancy disorder), the adaptation of the ANS to pregnancy is insufficient. Early detection of preeclampsia – which is a leading cause of perinatal morbidity and mortality – could allow for timely interventions that mitigate the burden of disease.
Owing to the association of preeclampsia with autonomic dysfunction, monitoring of maternal heart rate variability (mHRV) – a proxy measure for ANS activity – could aid in early detection of preeclampsia. A clear understanding of changes in mHRV in preeclampsia is necessary to facilitate this early detection. A systematic review by Moors et al. on this subject supported the hypothesis of a sympathetic overdrive in preeclampsia, which is associated with a parasympathetic withdrawal. However, the included studies in our review showed a large heterogeneity.
Furthermore, possible confounders remain for studies assessing mHRV in preeclamptic patients, such as the effect of routinely administered obstetric medications. Consequently, the MAMA-hart study has been set up to determine the effect of these medications on mHRV. This study was collaboratively planned within the e/MTIC ecosystem and will run at Máxima MC within the next few months. More information : www.ncbi.nlm.nih.gov/pubmed/32179490

Maarten van den Broek (WP4)
Project: Diagnosis and management of Atrial Fibrillation compounded by Obstructive Sleep Apnea
Our mission is to better understand the different OSA-related pathophysiological mechanisms, such as intrathoracic pressure swings, hypoxia and arousals, that initiate atrial fibrillation. This requires a smart cooperation between the Cardiology department of the Catharina Hospital and Centre for Sleep Medicine Kempenhaeghe for adequate patient selection and diagnostics. The subsequent analysis of the acquired multiparametric data is conducted at the Eindhoven Technical University, with the aid of Philips Research. And finally, the results of this research need to be implemented in daily clinical care at the Cardiology department of the Catharina Hospital.
OSA is a highly prevalent, often undiagnosed, modifiable risk factor for AF, as well as AF-related complications and treatment effectiveness. It is unclear which OSA-related pathophysiological mechanism, i.e. intrathoracic pressure shifts, hypoxemia or sympathovagal imbalance, plays the most dominant role, and a better understanding of these mechanisms could provide valuable information in future diagnostic and therapeutic strategies in this population.
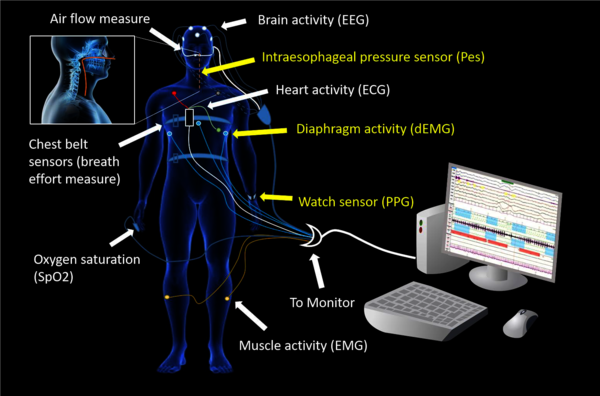
The primary objective is to assess the role of OSA-related pathophysiological mechanisms in the initiation of AF by a multi-parametric strategy that combines the estimated parameters. The main hypothesis is that intrathoracic pressure fluctuations are the predominant mechanism. The secondary objective is to validate a nonobtrusive sensing technology based on photoplethysmography and diaphragm electromyography measurements as surrogates for gold standard technology based on invasive intraoesophageal pressure measurement. For this, adult patients with paroxysmal AF with nocturnal onset and high risk of OSA will be studied in an observational study. Subjects are recruited from the AF outpatient clinic of the Catharina Hospital, and referred to Kempenhaeghe Centre for Sleep Medicine for a one-night full PSG, with the addition of dEMG and PPG. The acquired data will be analysed at the Eindhoven Technical University with the aid of Philips Research.
Arjet Nievergeld (WP5)
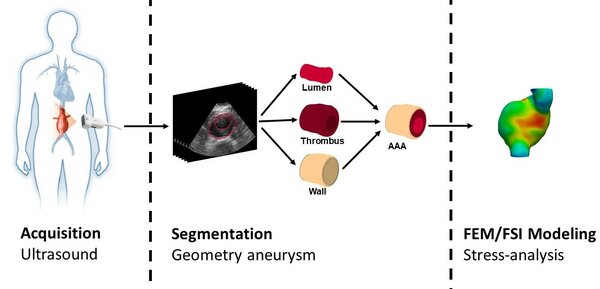
Project: Automated analysis of abdominal aortic aneurisms (AAAs) by means of ultrasound
An abdominal aortic aneurysm (AAA) is a localized dilatation of the aorta, which in case of rupture has a mortality rate of 80%. Current clinical guidelines of intervention are based on AAA diameter, which has been proven to be an inadequate criterion. Biomechanical models can improve the prediction of rupture risk in a more patient-specific way, using e.g. CT or ultrasound (US) imaging. However, CT requires the use of X-ray and nephrotoxic contrast agents. US overcomes the disadvantages of CT and adds temporal information on wall motion. Several studies have shown the feasibility of personalized modeling using US. It is hypothesized that intraluminal thrombus (ILT) has an effect on AAA rupture, presumably by lowering the peak wall stress. Therefore, it is necessary to include ILT in patient-specific models. Imaging ILT is challenging using US considering the low contrast. The objective of this study is to determine the patient-specific geometry of the AAA wall, ILT and lumen in 4-D US images for future finite element FSI modeling